The COVID-19 pandemic is showing no signs of slowing down even after 18 months. Therefore, the need for efficient treatments is a desperate one. Several scientists believe the ideal candidates can be found among existing drugs and repurposed to combat the SARS-CoV-2 coronavirus. Now, a new study has found that a commonly prescribed diabetes drug can prevent lung inflammation in COVID-19 patients.
According to the multi-institutional study, Metformin—an orally consumed diabetes drug—prevents pulmonary inflammation caused by COVID-19. The researchers identified the molecular mechanism behind the drug's anti-inflammatory activity using an animal model; thereby, confirming the link that was so far considered only a strong correlation by previous studies.
"The clinical studies were plagued by confounders that made conclusions hard to reach. There was some skepticism in their findings. And because metformin is an out-of-patent, low-cost drug, there is little impetus to conduct large-scale trials, which are quite expensive," said Dr. Michael Karin, corresponding author of the study, in a statement.
An Unexplained Correlation
Metformin is sold under the brand name 'Glucophage'. It is widely prescribed for the treatment of type 2 diabetes. Metformin acts by lowering the production of glucose in the liver and reducing blood sugar levels. This results in the improved response of the body to insulin. Scientists have observed that the drug also exhibits properties that are anti-inflammatory in nature. However, the workings behind this mechanism remained unknown.
Over the course of the pandemic, retrospective clinical studies have reported that in diabetic and obese patients—both of whom are in the high-risk category for COVID-19—who had been using Metformin before being hospitalized for the viral disease, a correlation with decreased severity and mortality was observed. Remarkably, no other drug used for controlling blood sugar levels was found to display such an effect.
These studies propounded that the anti-inflammatory activity of Metformin could be the reason behind the correlation with improved outcomes. The biggest drawback of the suggestion, however, was that the blood-glucose-lowering function of the Metformin had not been considered as a factor for the positive outcome in COVID-19 patients. None of the studies provided explanations or engaged in large-scale, randomized clinical trials that are essential for obtaining definitive answers.
Looking Into the Action of Metformin
In order to understand the fundamental mechanism behind Metformin's suggested role in reducing severity and mortality among COVID-19 patients, the team turned to mice models of acute respiratory distress syndrome (ARDS). ARDS is a potentially lethal condition where fluids accumulate in the air sacs (alveoli) of the lungs. This results in breathing difficulties and greatly limits the supply of oxygen to other essential organs in the body. The onset of ARDS is triggered by injuries or critical illnesses such as severe viral or bacterial infections.
Among hospitalized COVID-19 patients, ARDS is a prevalent cause of death. During the study, the authors administered Metformin to the mice before or after exposing them to bacterial endotoxin, a substitute for bacterial pneumonia. It was found that the dispensing of the drug led to the suppression of ARDS' onset and the reduction of its symptoms, along with a notable decrease in mortality among infected mice.
Importantly, it was observed that Metformin also inhibited the production of IL-1β (Interleukin 1 beta) and the gathering of inflammasome within alveolar macrophages (immune cells in the lungs). IL-1β is a cytokine. Cytokines are signaling proteins that moderate the immune system by attracting immune cells to the area of infection.
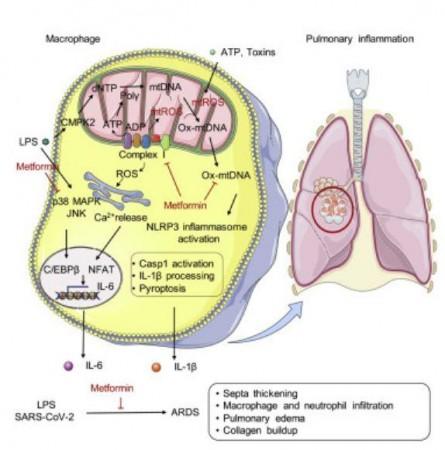
Among patients with severe COVID-19, the signaling mechanism is hindered and a haywire response of the immune system or a 'cytokine storm' causes damage to healthy tissues in several vital organs including the lungs. Inflammasome, a large protein complex, regulates the production of IL-1β. Some of the co-authors of the study had previously discovered that there was an increased presence of inflammasome in the lung tissues of patients who succumbed to COVID-19.
Discovery of Crucial Mechanism
After further examinations, the authors were able to confirm that Metformin indeed inhibited the activation of the inflammasome and averted pulmonary inflammation in mice due to the SARS-CoV-2 infection. Through cell culture studies involving macrophages, the authors discovered the fundamental mechanism by which Metformin wields anti-inflammatory activity: decreased production of ATP (Adenosine triphosphate) by the mitochondria.
ATP is an energy-carrying molecule that the mitochondria use to store energy for cellular processes. Though crucial for cellular functions, the lessened production of ATP in liver cells is responsible for Metformin's glucose-lowering effect. Decreased quantities of ATP within macrophages were found to inhibit mitochondrial DNA synthesis, which is a crucial step in the activation of an inflammasome known as NLRP3. Further research revealed that the removal of damaged mitochondria led to a reduction in NLRP3 inflammasome activity and decreased inflammation.
The scientists also established that the specific interference with the synthesis of mitochondrial DNA in macrophages due to the removal of an enzyme called CMPK2 (cytidine monophosphate kinase 2) inhibited the production of IL-1β (but not IL-6, another cytokine) and prevented the onset of ARDS. "These experiments strongly suggest that improved delivery of metformin or CMPK2 inhibitors into lung macrophages can provide new treatments for severe COVID-19 and other forms of ARDS," expressed Dr. Elsa Sanchez-Lopez, co-senior author of the study.
According to the authors, the findings of the study suggest that metformin shows potential for being used for treating a wide range of cardiovascular and neurodegenerative diseases where the activation of NLRP3 inflammasome is a crucial factor. "Inhibition of inflammasome activation may also account for the poorly explained anti-aging effect of metformin," concluded Karin.

















