As countries such as India are battling the COVID-19 pandemic on one side, their health infrastructure is being pushed to its limits by the concurrent outbreaks of diseases such as the Black fungus infection among SARS-CoV-2 coronavirus patients. Scientists now report that COVID-19 is creating ideal conditions for the emergence of a 'superfungus'—Candida auris.
According to a new study conducted in Brazil (led by the São Paulo Research Foundation), Candida auris infections among severe COVID-19 patients may lead to increased mortality. The study found that the fungus—that is developing drug resistance at a phenomenal rate—may be able to persist in hospitals despite sanitary measures and infect resident patients especially those admitted to intensive care units.
"The species quickly becomes resistant to multiple drugs and isn't very sensitive to the disinfectants used by hospitals and clinics. As a result, it's able to persist in hospitals, where it colonizes health workers and ends up infecting patients with severe COVID-19 and other long-stay critical patients," said Dr. Arnaldo Colombo, lead author of the study, in a statement.
A 'Superfungus' Among Pathogenic Fungi
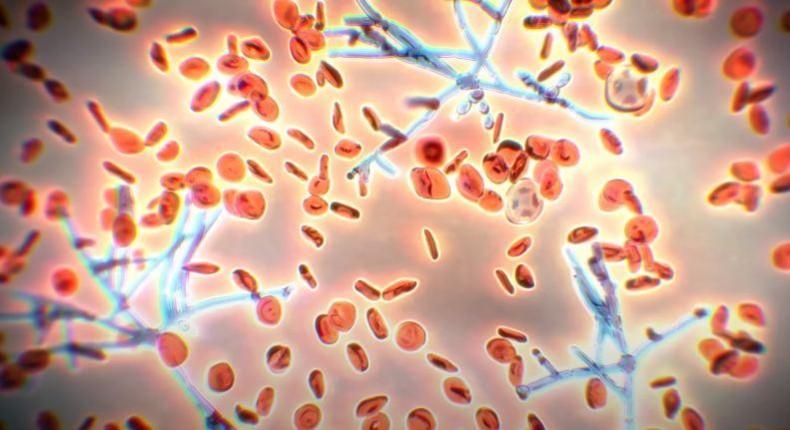
Fungi are naturally found across different habitats including on and within flora and fauna. Candida, which belongs to the genus of yeasts, often shares a symbiotic relationship with host cells and is found on their mucosal membranes, including human ones. Some strains of Candida (except C.auris) form an integral part of the human gut microbiota. However, in the event of immunosuppression—repression of the immune system—or a breach in the mucosal membrane barriers, or imbalances within the organism, Candida can have pathogenic effects.
Species such C. albicans can cause Candidiasis or thrush (which affects the mouth and the vagina) and skin infections. In some extremes cases, the entry of the fungus into the bloodstream can result in candidemia, an invasive form of candidiasis that is similar to bacteria-caused sepsis. The incursion of the bloodstream and the immune system's aggressive response to the fungus can result in acute damage to several vital organs and even death. Studies have found that among candidemia patients infected with C. auris—which was first isolated in Japan in 2009—the mortality rate can be as high as 60 percent.
For the study, the authors investigated the first two confirmed cases—a 59-year-old male and 74-year-old female—of C. auris infection at a hospital in the Brazilian city of Salvador in December 2020. Both the patients were admitted to the same COVID-19 intensive care unit. According to the authors, other cases of C. auris were also reported later in the same hospital with varying degrees of harm caused.
Local Emergence of the Fungus
The authors found that in antifungal susceptibility testing of samples from the two patients, there was minimal inhibition when exposed to common antifungal drugs such as anidulafungin, amphotericin B, fluconazole, and voriconazole that are used to treat candidiasis. When they conducted microsatellite typing—analysis of genetic markers—it was learnt that the strains were clonal and belonged to the South Asian clade or lineage of C. auris.
So far, five clades of C. auris have been identified across the world. According to Dr. Colombo, the lineage isolated in Salvador closely resembled the original Asian model than the variants detected in other South American countries; thereby, suggesting a second independent entry into the continent by the superfungus.
The authors noted that several travel restrictions were in effect in Brazil at the time due to the ongoing COVID-19 pandemic. Also, neither of the patients had any overseas travel history or relatives sick with the pathogen. This led the team to hypothesize that this particular species was introduced several months before the identification of the first case, and/or, arose locally in the Salvador area.
"Nine other C. auris patients have since been diagnosed at the same hospital, some colonized [with the fungus in their organism but not doing harm] and others infected. No other cases have been reported in Brazil, but there are grounds for concern. We're monitoring the evolutionary characteristics of C. auris isolates from patients at the hospital in Salvador, and we've already found samples with reduced sensitivity to fluconazole and echinocandins," explained Dr. Colombo.
COVID-19 and the Rise of C. auris
Co-infections with other pathogens such as mucormycetes (that cause black fungus) infections have been widely reported. Patients with COVID-19 become susceptible to C. auris due to numerous factors. These include extended hospital stays, central venous and urinary catheters (enabling invasion of the bloodstream), and extensive use of antibiotics and steroids (which causes immunosuppression and disruption of gut microbiota). The authors note that the often unjustified prescription of antibiotics along with invasive procedures leaves COVID-19 patients vulnerable to 'superinfections'.
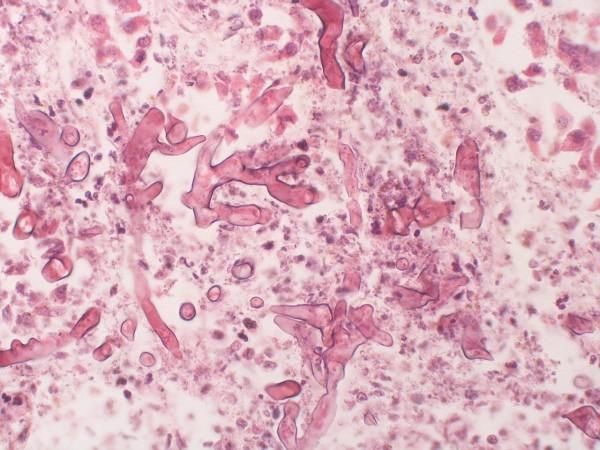
Dr. Colombo noted that the emergence of C. auris has been reported in several countries during the course of the pandemic, which makes monitoring and controlling of hospital-acquired infections crucial. The study states that the COVID-19 pandemic "may be accelerating the introduction and/or spread of C. auris in previous C. auris-free hospital environments". In an effort to monitor, the scientists have been receiving samples from the clade isolated at the hospital in Salvador for testing its susceptibility to antifungal drugs.
Explaining the basis of C. auris's resistance to medications, Dr. Colombo said, "The mechanism that enables the species to develop drug resistance isn't enzymatic degradation, as in so many bacteria that are resistant to antibiotics. The fungus develops structural modifications in the proteins to which the drug binds to inhibit cell wall synthesis [glucan synthase in the case of echinocandins], which is key to its survival. We're seeing this phenomenon happen here in Brazil."

















