With potent virulence and transmissibility, the SARS-CoV-2 virus is one of the deadliest pathogens to be encountered in recorded history. Scientists have reiterated that other than hygienic measures, distance between individuals is the best defense against its spread. However, the latter is difficult within a household and presents challenges in the event of a member contracting the coronavirus infection. Now, a new study has stated that the infection rate among housemates can be over 30 percent.
Researchers from the University of North Carolina found that the secondary attack rate of the infection within the household of COVID -19 positive individuals was 32 percent. The study also learnt that this rate was disproportionately higher—51 percent—among minority households of color where household density served as a crucial factor.
"Our data also suggest that those infected with a high viral load are not only more likely to transmit virus to other household members, but that they may seed other high-viral load infections, putting the entire household at higher risk for more severe illness," wrote the authors. The research was published in the journal Clinical Infectious Diseases.
Examining Spread within Households

Since the onset of the COVID-19 pandemic, it has been observed that the virus can sweep through families and communities with lethal swiftness. Such large-scale spreads have been a concern in poor and heavily populated communities where the density of people is higher. The current observational study was carried out between April and October 2020. 100 individuals who had tested positive (index cases) for COVID-19 around the city of Raleigh, North Carolina's capital were followed by the team.
Additionally, 208 household members were also monitored; a total of 102 households. The researchers defined a household member as someone who lived in the same living space as the infected individual at the time of their diagnosis. Some participants were excluded due to factors such as evidence of prior infection, non-completion of follow-up, and being infected through the same common source as the primary case. The study population was trimmed down to 91 households comprising 176 members.
Other housemates were tested weekly using PCR nasal swabs after the first COVID case, or in the fourth week using a seroconversion antibody test. Except for 73 household members who had already tested COVID positive before the researchers visited their homes, the secondary attack rate among household contacts was found to be 32 percent (33/103).
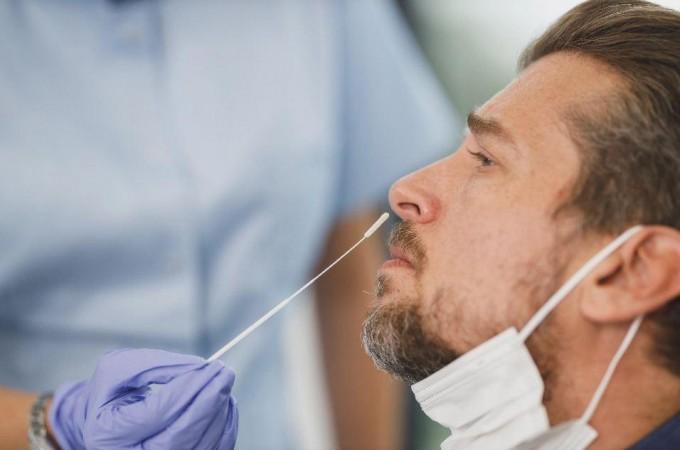
"We think this number is actually much higher. Sometimes we were getting to households to test people four or five days after the initial COVID-positive person showed symptoms. By that time a lot of household members were already infected. But because that infection happened before we got there, we couldn't include it in our data," said Dr. Jessica Lin, senior author of the study, in a statement.
Viral Load Matters
Most of the secondary cases occurred within the first week of the primary positive COVID test. It was found that the secondary cases had similar nasopharyngeal viral loads (the quantity of virus in the nose and throat). Dr. Lin noted that this study was conducted before the Delta variant became prevalent in the US. Therefore, the current rate of secondary attacks could be higher she suggested.
"This means the viral load of the index case matters. A higher viral load means it's more likely that there will be secondary transmission in a household, and viral load is also an indication of how sick a person could get from the virus," explained Dr. Lin, who is an assistant professor in the UNC Department of Medicine, Division of Infectious Diseases at the UNC School of Medicine.
Role of Living Density
Another area that the study focused on as a factor determining the spread of infection within a household was living density (i.e) the concentration of people living in a household. Among the participants who were recruited for the study, 44 percent identified as non-white or Hispanic.
The authors observed that in minority households, the probability of experiencing a higher living density was more. Such households were found to have a larger risk of secondary infections than white households. The secondary attack rate rose to 51 percent in these households as against 32 percent for the total study population.
"It's very difficult to follow public health guidelines in some living situations. If you have multiple people and generations sharing common areas or bedrooms, or say you are a single parent, it becomes nearly impossible to isolate or even physical distance," commented Dr. Lin.
Vaccination to Mitigate Risk
So how can the chances of secondary infection within a household be reduced? Dr. Lin said that vaccination is the answer. When more number of members in a household are vaccinated, the chances of secondary COVID infections occurring are lower.
Even if only one person is vaccinated, and this person is the first to contract the infection, being vaccinated helps. This is because it is has been shown that a vaccinated individual is most likely to harbor a lower viral load. As a result, the chances of infecting other members of the household are lessened.
"Household transmission really is the main place where most people are getting COVID. It's spreading from their family and friends, people that are in their bubble and they feel safe with. When you get vaccinated, you aren't just protecting yourself, you're protecting those important people around you," concluded Dr. Lin.














